Introduction
 A painful knee can severely affect your ability to lead a full active life. Over the last twenty five years, major advancements in artificial knee replacement have improved the outcome of the surgery greatly. Artificial knee replacement surgery is becoming more and more common as the population of the world begins to age.
A painful knee can severely affect your ability to lead a full active life. Over the last twenty five years, major advancements in artificial knee replacement have improved the outcome of the surgery greatly. Artificial knee replacement surgery is becoming more and more common as the population of the world begins to age.
Causes
There are many conditions that can result in degeneration of the knee joint. Osteoarthritis is the most common cause that patients need to undergo knee replacement surgery. This condition is commonly referred to as “wear and tear arthritis”. Osteoarthritis can occur with no previous history of injury to the knee joint – the knee simply “wears out”. There may be a genetic tendency in some people that increases their chances of developing osteoarthritis.
The major problem in osteoarthritis is that the cartilage (the articular cartilage) on the surface of the bone inside the joint wears away. This results in bone rubbing against bone, the slick protective surface of the articular cartilage is absent. This causes pain.
Abnormalities of knee joint function resulting from fractures of the knee, torn cartilages and torn ligaments can lead to degeneration many years after the injury. The mechanical abnormality leads to excessive wear and tear – just like the out of balance tire that wears out too soon on your car. For more information of these injuries, see A Patient’s Guide to Knee Problems
Symptoms
The symptoms of a degenerative knee joint usually begin as pain while bearing weight on the affected knee. You may limp and the knee may become swollen with fluid. The degeneration can lead to a reduction in the range of motion of the affected knee – the knee bends less than normal and may lose the ability to completely straighten out. Bone spurs will usually develop and can be seen on xray. Finally, as the condition becomes worse, the pain may be present all the time and may even keep you awake at night.
Diagnosis
The diagnosis of a degenerative knee starts with a complete history and physical examination by your doctor. X-rays will be required to determine the extent of the degenerative process and may suggest a cause for the degeneration. Other tests may be required if there is reason to believe that other conditions are contributing to the degenerative process. Blood tests may be required to rule out systemic arthritis (such as Rheumatoid Arthritis) or infection in the knee.
Medical Treatment
Not all degenerative knee conditions require a knee replacement as the initial treatment. Your doctor may suggest several alternative treatments to put off the decision for replacing the knee as long as possible. Using a cane may help alleviate some of your pain and allow you to walk more comfortably. Anti-inflammatory medications may reduce the inflammation from the arthritis and reduce your pain.
Surgery
Most degenerative problems will finally require replacement of the painful knee with an artificial knee replacement. The decision to proceed with surgery should be made jointly by you and your doctor only after you feel that you understand as much about the procedure as possible.
Once the decision to proceed with surgery is made, there are several things that may need to be done. Your orthopedic surgeon may suggest a complete physical examination by your medical or family doctor. This is to ensure that you are in the best possible condition to undergo the operation. You may also need to spend time with the Physical Therapist who will be managing your rehabilitation after the surgery. The therapist will be able to begin the teaching process before the surgery to ensure that you are ready for the rehabilitation afterwards.
One purpose of the preoperative visit is to record a baseline of information. This includes your measurements of your current pain levels, functional abilities, the presence of swelling, and the available movement and strength of each knee.
A second purpose of the preoperative visit is to prepare you for your upcoming surgery. You’ll begin to practice some of the exercises you’ll use just after surgery. You’ll also be trained in the use of either a walker or crutches. Whether the surgeon used a cemented or noncemented approach will determine how much weight you’ll be able to apply through your foot while walking Finally, an assessment will be made of any needs you’ll have at home once you’re released from the hospital.
Finally, you may be asked to donate some of your own blood before the operation. This blood can be donated 3-5 weeks before the operation and your body will make new blood cells to replace the loss. At the time of the operation, you will receive your own blood back from the blood bank in case you need to have a blood transfusion.
The Artificial Knee
There are two major types of artificial knee replacements:
- Cemented Prosthesis
- Uncemented Prosthesis
Both are still widely used. In many cases a combination of the two types are used. The patellar(kneecap) portion of the prosthesis is commonly cemented into place. The choice to use a cemented or uncemented artificial knee is usually made by the surgeon based on your age, your lifestyle, and the surgeons experience.
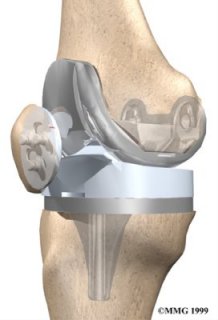
Each prosthesis is made up of four parts:
- The tibial component (bottom portion) replaces the top of the lower bone, the tibia.
- The femoral component (top portion) replaces the two femoral condyles and the groove where the patella runs.
- The patellar component (kneecap portion) replaces the joint surface on the bottom of the patella that rubs against the femur in the femoral groove.
- The femoral component is made of metal. The tibial component is usually made up of two parts – a metal tray that is attached directly to the bone and a plastic spacer that provides the bearing surface. The plastic used is very tough and very slick – (so slick and tough that you can ice skate on a sheet of the plastic with out much damage to the material).
A cemented prosthesis is held in place by a type of epoxy cement that attaches the metal to the bone. An uncemented prosthesis has a fine mesh of holes on the surface that allows bone to grow into the mesh and attach the prosthesis to the bone.
The Operation
You can download a surgical animation showing the steps involved in replacing a diseased knee with an artificial knee. The steps involved in replacing the knee begin with making an incision on the front of the knee to allow access to the knee joint. There are several different approaches used to make the incision, usually based on the surgeon’s training and preferences.
Shaping the Distal Femoral Bone
Once the knee joint is entered, a special cutting jig is placed on the end of the femur. This jig is used to make sure that the bone is cut in the proper allignment to the leg’s original angles – even if the arthritis has made you bowlegged or knock-kneed. The jig is used to cut several pieces of bone from the distal femur so that the artificial knee can replace the worn surfacs with a metal surface.
Preparing the Tibial Bone
Attention is then turned towards the lower bone, the tibia. The top of the tibia is cut using another of jig that ensures the alignment is satisfactory.
Preparing the Patella
The undersurface of the patella is removed.
Placing the Femoral Component
The metal femoral component is then placed on the femur. In the uncemented variety of femoral component, the prosthesis is held on the end of the bone by the fact that the end of the bone is tapered, and the metal prosthesis is cut so that it matches the taper almost exactly. Driving the metal component onto the end of the bone holds the component in place by friction. In the cemented variety, an epoxy cement is used to attach the metal prosthesis to the bone.
Placing the Tibial Component (metal tray)
The metal tray that will hold the plastic spacer is attached to the top of the tibia. The metal tray is either cemented into place, or held with screws if the component is of the uncemented variety. The screws are primarily used to hold the tibial tray in place until the bone grows into the porous coating. (The screws remain in place and are not removed.)
Placing the Tibial Component (plastic spacer)
The plastic spacer is then attached to the metal tray of the tibial component. If this component should wear out while the rest of the artificial knee is sound, it can be replaced – a so called retread.
Placing the Patellar Component
The patella button is usually cemented into place behind the patella.
The Completed Knee Replacement
X-ray from the side
X-ray from the front
Rehabilitation
While you are in the hospital:
- Range of Motion
- Ambulation
- Exercises
The physical therapist will schedule your first inpatient visit shortly after surgery. Treatment will address the range of motion in the knee. Gentle movement will be used to begin to help you regain both the bending and straightening of the knee. If you are using a CPM (continuous passive motion) device, it will be checked for alignment and settings. Next, you’ll go over your exercise regimen. When you are stabilized, your therapist will assist you up for a short outing using your crutches or your walker. Treatment will proceed on a one to two time per day basis. You’ll be on your way home when you can demonstrate a safe ability to get in and out of bed, walk up to 75 feet with your crutches or walker, get up and down flight of stairs and access the bathroom. It is also important that you regain a good muscle contraction of the upper thigh muscle (quadriceps) and that you gain improved knee range of motion.
After you leave the hospital:
Home health needs
Once discharged from the hospital, your therapist will likely see you for in home treatment. This is to ensure you are safe in and about the home. You should be seen for at least one visit for the safety check and to review your exercise program. In some cases you may require up to three visits at home before beginning outpatient physical therapy.
As you progress:
Outpatient progression
Welcome to outpatient physical therapy. Several key areas will be addressed. Your therapist may choose one or more modalities such as heat, ice, or electrical stimulation to help reduce persistent swelling or pain. Continue to use your walker or crutches. If you had a cemented procedure, you’ll advance the weight you place through your sore leg as much as you feel comfortable. If yours was a noncemented procedure, place only the toes down until you’ve had a follow-up x-ray and your doctor or therapist directs you to advance the amount of weight through your leg (usually by the 5th or 6th week postoperatively). Range of motion exercises and techniques will be used to help you regain full bending and straightening of the knee. An exercise program will be developed including strengthening, balance, and endurance, and functional activities. Your strengthening program will address key muscle groups including the buttock and hips, thigh, and calf muscles. When you are safe in putting full weight through the leg, several balance exercises can be chosen to further stabilize and control the knee. Endurance can be achieved through stationary biking, lap swimming, and using and upper body ergometer (upper cycle). Finally, a select group of exercises can be used to simulate day-to-day activities, like going up and down steps, squatting, raising up on your toes, and bending down. Specific exercises may then be chosen to simulate work or hobby demands.
Complications
As with all major surgical procedures, complications can occur. Some of the most common complications following knee replacement are:
- Thrombophlebitis
- Infection
- Stiffness
- Loosening
This is not intended to be a complete list of the possible complications, but are the most common.
Thrombophlebitis
Thrombophlebitis, sometimes called Deep Venous Thrombosis (DVT), can occur after any operation, but is more likely to occur following surgery on the hip, pelvis, or knee. DVT occurs when the blood in the large veins of the leg forms blood clots within the veins. This may cause the leg to swell and become warm to the touch and painful. If the blood clots in the veins break apart, they can travel to the lung, where they get lodged in the capillaries of the lung and cut off the blood supply to a portion of the lung. This is called a pulmonary embolism. (Pulmonary = lung, embolism = fragment of something traveling through the vascular system). Most surgeons take preventing DVT very seriously. There are many ways to reduce the risk of DVT, but probably the most effective is getting you moving as soon as possible!
Some of the commonly used preventative measures include:
- Pressure stockings to keep the blood in the legs moving.
- Medications that thin the blood and prevent blood clots from forming.
Infection
Infection can be a very serious complication following an artificial joint. The chance of getting an infection following artificial knee replacement is probably somewhere around 1%. Some infections may show up very early – before you leave the hospital. Others may not become apparent for months, or even years, after the operation. Infection can spread into the artificial joint from other infected areas. Your surgeon may want to make sure that you take antibiotics when you have dental work, or surgical procedures on your bladder and colon to reduce the risk of spreading germs to the joint.
Stiffness
In some cases, the ability to bend the knee does not return to normal after an artificial knee replacement. Many orthopedic surgeons are now using a machine known as a CPM machine (Constant Passive Motion) immediately after surgery to try and increase the range of motion following artificial knee replacement. Other orthopedic surgeons rely on physical therapy beginning immediately after the surgery to regain the motion. It is not clear which is the best approach. Both approaches have benefits and risks, and the choice is usually made by the surgeon based on his experience and preferences.
To be able to use the leg effectively to rise from a chair, the knee must bend at least to 90 degrees. A desirable range of motion should be greater than 110 degrees. Balancing of the ligaments and soft tissues (during surgery) is the most important determining factor in regaining an adequate range of motion following knee replacement, but sometimes increasing scarring after surgery can lead to an increasingly stiff knee. If this occurs, your surgeon may recommend taking you back to the operating room, placing you under anesthesia once again, and forcefully manipulating the knee to regain motion. Basically, this allows the surgeon to breakup and stretch the scar tissue without you feeling it. The goal is to increase the motion in the knee without injuring the joint.
Loosening
The major reason that artificial joints eventually fail continues to be a process of loosening where the metal or cement meets the bone. There have been great advances in extending how long an artificial joint will last, but most will eventually loosen and require a revision. Hopefully, you can expect 12-15 years of service from an artificial knee, but in some cases the knee will loosen earlier than that. A loose prosthesis is a problem because it causes pain. Once the pain becomes unbearable, another operation will probably be required to revise the knee replacement.